Coming to terms with having low milk supply and accepting that supplementation is going to have to be part of your breastfeeding journey can often be very difficult for women to come to terms with. One of my clients wrote about her experience of realising she had insufficient glandular tissue, and the practical and emotional challenges that having the condition presented her with. She writes beautifully, and with such honesty, I’m just delighted she has given me permission to share her story here.
“Breastfeeding was always something that I was going to do. It wasn’t even a decision I had to make; I was just doing it. I had spent my life knowing this one fact and knowing I was breastfed, watching my sisters breastfeed their babies and becoming a midwife simply cemented my dedication to my own breastfeeding journey. When I got pregnant, I used to tell my husband that the thing I was looking forward to most was breastfeeding my little babe. I was excited to feel the latch, to see my milk come in and to know I was nourishing my baby. I could not wait for the sleepless cluster-feeding nights! I felt such a deep sense of connection between my body and breastfeeding as an experience.
Around 20 weeks into my pregnancy, I asked a lactation consultant in the hospital I work in as a midwife if I should be concerned that I hadn’t experienced much breast changes in early pregnancy, only some tenderness/tingling/changes in temperature but she reassured me that even minor changes ‘count’. It really never occurred to me to consider my history of polycystic ovarian syndrome (PCOS) or my breast type/tissue. I know, not very smart of a midwife!! But honestly, I just had it solidified in my head that I was exclusively breastfeeding and that was that. So much so that I went back and forth about buying an emergency supply formula before I had my baby. But the midwife in me convinced myself to buy a 24-hour supply just in case we ran in to weight loss or jaundice issues!
At 37 weeks, I decided to start antenatal expression to have a supply of colostrum for the initial days if needed. It was back and forth for me whether I would end up needing a c-section and I knew that no formula was to pass my baby’s lips if we were to be separated for any reason. In fact I had my husband under strict instructions to keep saying so if I wasn’t in a position to advocate that for myself! In the end I had a very fast and intense vaginal delivery, with a placenta that was more stubborn to deliver than the baby was! I needed some oxytocin to help the placenta to deliver.
Everything else seemed fairly ‘normal’ to me. My baby girl latched on within an hour of birth and was feeding for good periods of time regularly from then on. I gave her the expressed colostrum intermittently from the day after birth because her urine was a little concentrated. We got home after 24 hours and feeding was going well.
By day 4 I was concerned as I had no signs of milk coming in other than a slight change in milk colour. I mentioned it to the community midwife visiting me who reassured me to keep feeding and the milk would come in the next 24-36hrs. I was also concerned that baby’s urine was still concentrated and she hadn’t had a bowel movement since the day of birth. We decided to give some small formula top ups overnight to help with that. I was still thinking I was going to wake up the next day pouring with milk!! Day 5 and there was still no change. The community midwife made a passing comment about my breast shape and difficulty establishing a supply. Despite my reluctance the community midwife, my husband and midwife friends convinced me to increase the formula amounts and I got in touch with a lactation consultant, Caoimhe.
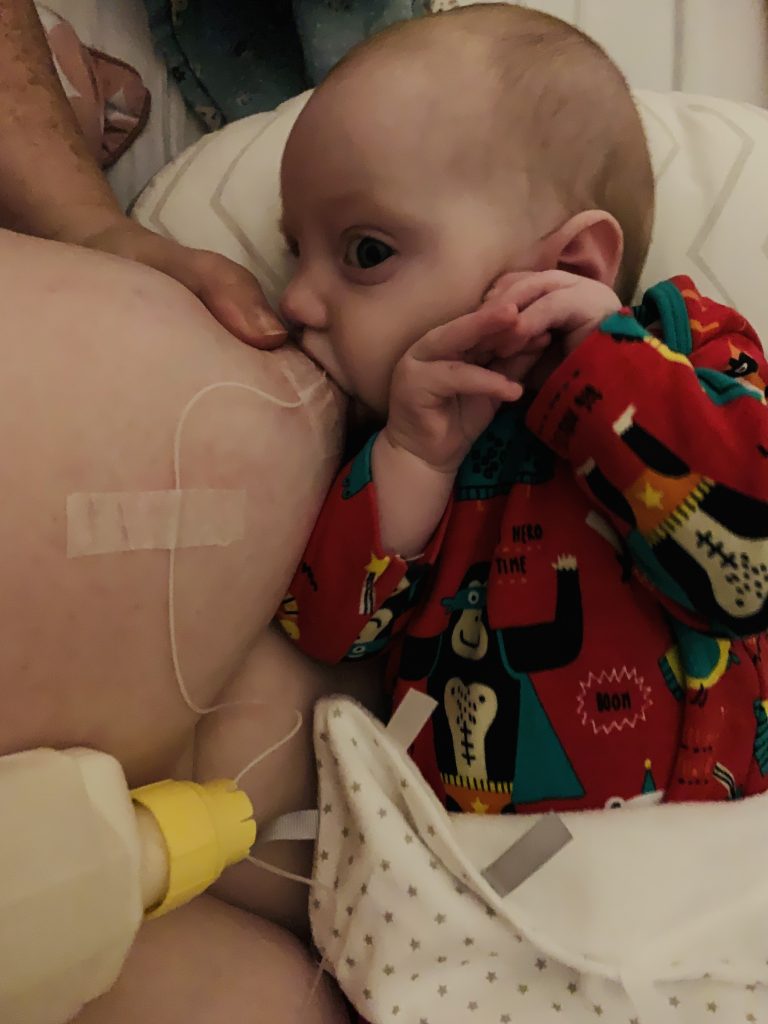
I had a sense that things were not as they should be and my conversation with Caoimhe brought me to the full realisation that my long-term vision of exclusive breastfeeding was suddenly looking very cloudy. Caoimhe supplied us with the equipment needed to create a ‘homemade’ supplementary nursing system – because I was adamant to keep my daughter at the breast as much as possible and because top ups via a bottle seemed to be disrupting her skills of latching on. She also gave us a video tutorial of how to supplement at the breast using a tube and told us about the Medela supplemental nursing system (SNS) version. While I sobbed like I have never sobbed before into week 2 of being a mum, the SNS was giving me something I couldn’t appreciate yet – a continuation of my breastfeeding journey. I didn’t even know such a thing as an SNS existed and all of a sudden here I was fiddling around with one at 3am just to keep my breastfeeding going. I battled with waves of grief that breastfeeding was not working out for us the way I had dreamed it would. For weeks I looked at the SNS as the evil formula delivery system that was interrupting my plan for exclusive breastfeeding whilst also somehow being grateful for this saving grace allowing me to maintain that incredible embodied connection to my daughter that I was unwilling to relinquish.
Practically, the SNS has its pros and cons. It can be super fiddly and a pain in the arse when the valve seal goes mysteriously and you end up with formula pouring down your front. The ‘homemade’ version (a nastogastric tube and bottle) wasn’t for us as my daughter is quite the eater and despite holding it at the lowest possible point, she had it emptied in minutes! The Medela SNS with valve and different size tubing allows me to more carefully control her eating and enables her to suck more effectively at the breast. And that had a huge impact on my supply! In week 2 I was able to yield 3-10mls of breastmilk from a double pump session, now that is 30-40mls. I know that is in large part down to the SNS encouraging my daughter to feed more effectively. I vowed early on to make it our ‘normal’ that the SNS was just part of our breastfeeding and I’m lucky that introducing it on day 5/6 meant that my daughter knows no different. I have also had to push myself to use it out and about. I think having to set it up (tie it around the neck and tape tubes to the breast) can be awkward and you’re more exposed initially which some people might find prohibitive but I refuse to let that stop me. I am trying to give myself as much of that original dream vision as I can so the SNS comes with us wherever we go and I tell as many people as want to listen about my special extra milk buddy. All my nieces and nephews think it’s very cool!! Emotionally my relationship with the SNS remains complex. I love it because it means that we are still breastfeeding and that my daughter is getting good intake of breastmilk. I do still resent having to use it, but I think that will go in time. I would definitely encourage another mum to try it if she needed it, and I will be going back to being a better midwife at the end of my maternity leave because of this experience! Ultimately, it has been a hugely positive experience. Challenging yes, but rewarding too!“